Pharmacy
Oklahoma Complete Health is committed to providing appropriate, high-quality, and cost-effective drug therapy to all Oklahoma Complete Health members. Oklahoma Complete Health covers prescription medications and certain over-the-counter medications with a written order from an Oklahoma Complete Health provider. The pharmacy program does not cover all medications. Some medications may require prior authorization, and some may have limitations. Other medically necessary pharmacy services are covered as well. Oklahoma Complete Health follows the State of Oklahoma’s preferred drug and prior authorization criteria.
Use our Medicaid Preferred Drug List to find more information on the drugs that are covered.
Please refer to https://oklahoma.gov/ohca/providers/types/pharmacy/pharmacy.html for the most up-to-date lists of brand required medications, covered over-the-counter products, and diabetics supplies.
Please refer here: https://oklahoma.gov/ohca/providers/types/pharmacy/prior-authorization/2026.html for 2026 clinical criteria regarding medications needing prior authorizations.
If your pharmacy is experiencing a rejection & need an immediate override, please call our pharmacy helpdesks (open 24/7) at 1-833-750-3660 (SoonerSelect) or 1-833-750-3682 (Children's Specialty Plan). Please reach out directly to our local pharmacy team at oklahoma_complete_health_pharmacy@centene.com regarding general pharmacy questions or escalations.
Medication Prior Auth Search
Please utilize our Preferred Drug List posted above or our search tool function to determine if a medication requires a prior authorization, which tier the medication is in, or if the medication has step therapy, age, or quantity limits
Express Scripts, Oklahoma Complete Health’s PBM, processes pharmacy claims and supports pharmacy enrollment in our network. Information to contact Express Scripts for pharmacy enrollment is available online at this link: https://www.esiprovider.com/ This is an external link that will take you outside the Oklahoma Complete Health website.
For Application Assistance, Document Inquiries or if you have questions in regards to filling out your online application, please contact Express-Scripts at PBMProviderOperations@express-scripts.com.
Please include your pharmacy’s NCPDP in the email subject line.
Pharmacy Processing Information:
RxBIN 003858
RxPCN MA
RxGroup 2HFA
ID Numbers will remain the same as Medicaid ID#
Maximum Allowable Cost Pricing Information
Pharmacies across Express Scripts pharmacy network can log into ESI’s portal for MAC pricing information
https://prc.express-scripts.com/frontend/prcportal/#/index
Please refer here: https://oklahoma.gov/ohca/providers/types/pharmacy/prior-authorization/2025.html for 2025 clinical criteria regarding medications needing prior authorizations.
Additional Criteria
| Duplicate Therapy | 1.25 |
| Oklahoma Clinical Care Guidelines Atypical Antipsychotic Use for Members Under the Age of 5 | 4.24 |
| Request for 3rd Brand Name Fill | 2.25 |
| Stimulant Use for Members Under the Age of 5 | 4.24 |
| Antipsychotic & Stimulant Medications in Children under 5 Years | 3.25 |
| Guideline Name | Guideline # | Approved Version |
| 72 Hour Emergency Supply Of Medication | CC.PHAR.01 | 2025 Q1 |
| Approval of Brand-Name Override | CC.PHAR.02 | 2025 Q3 |
| Conflict of Interest and Confidentiality Agreement for Pharmacy and Therapeutics Committee Membership | CC.PHAR.17 | 2025 Q2 |
| Early and Periodic Screening, Diagnostic, and Treatment Benefit for Pediatric Members | CP.PMN.234 | 2025 Q2 |
| Lost, Stolen, Spilled or Broken Medication | CC.PHAR.05 | 2025 Q2 |
| Medicaid Preferred Drug List Audit Support | CC.PHAR.22 | 2024 Q4 |
| No Coverage Criteria, Recent Label Changes Pending Clinical Policy Update | CP.PMN.255 | 2024 Q4 |
| Off-Label Use | CP.PMN.53 | 2024 Q4 |
| Pharmaceutical Management | CC.PHAR.07 | 2025 Q3 |
| Pharmacy & Therapeutics Committee | CC.PHAR.13 | 2025 Q3 |
| Pharmacy and Therapeutics Committee Member Documentation and Tracking | CC.PHAR.16 | 2025 Q2 |
| Pharmacy Operations | CC.PHAR.23 | 2025 Q2 |
| Precision Drug Action Committee | CC.PHAR.21 | 2025 Q3 |
| Provider Requests for Pharmacy Profiles | CC.PHAR.11 | 2024 Q4 |
| Quantity Limit Override and Dose Optimization | CP.PMN.59 | 2024 Q4 |
| Split-Fill Program | CC.PHAR.24 | 2025 Q1 |
| Vacation Overrides | CC.PHAR.19 | 2025 Q2 |
Pharmacy Services reviews prior authorizations. CoverMyMeds is the fastest and easiest way to review, complete and track PA requests. Our electronic prior authorization (ePA) solution is HIPAA-compliant and available at no cost to providers and their staff.
To use COVER My MEDs please see: https://www.covermymeds.com/main/prior-authorization-forms/ This is an external link that will take you outside the Oklahoma Complete Health website.
OR CALL 1-833-331-1515 (SoonerSelect) or 1-833-655-0896 (SoonerSelect Children’s Specialty Program)
Prior Authorization Request Form for Most Prescription Medications (PDF)
Step Therapy Exception Request Form (PDF)
Prior Authorization Request Form- Atypical Antipsychotics for Children under the age of 5 (PDF)
Prior Authorization Request Form- Stimulants for Children under the age of 5 (PDF)
Check if CPT code requires authorization – https://www.oklahomacompletehealth.com/providers/preauth-check.html
Submit prior authorization via Availity-https://www.availity.com/essentials
Members may receive up to a 90-Day supply of certain maintenance medications pursuant to the State of Oklahoma’s maintenance drug program.
Maintenance Medications Up to 90 Days. link: https://oklahoma.gov/ohca/providers/types/pharmacy/maintenance-drug-list.html This is an external link that will take you outside the Oklahoma Complete Health website.
To find a pharmacy that is in the Oklahoma Complete Health network, you can use the Find a Provider tool
Specialty drugs used to treat complex, chronic conditions are generally filled at specialty pharmacies due to the storage, handling and requirements to dispense them. Pharmacies who accept all terms and conditions of these products and of our network may dispense these drugs. OHCA has implemented a limited specialty network for hemophilia. Pharmacies who would like to be considered in network for hemophilia will need to contact OHCA.
To protect the health of our members, Oklahoma Complete Health has a pharmacy lock-in program. This is for members who abuse or misuse prescription drugs. Members are assigned to one pharmacy and one doctor. Members may change your doctor or pharmacy one time a year unless you have a special situation like moving. If members are placed in the program, they may be enrolled for a minimum of two years. We will review enrollment at least every year. Members and providers also have the option to appeal being placed in the lock-in program.
Historically there have been some over the counter products on the state's formulary; however, pharmacies don't always have them in stock or the products our members need aren't covered. Therefore, we have implemented an Over-the-Counter Product Value Add Benefit. The benefit is $30 per member per quarter. Our members can view the full catalog of items on our website and can order online (cvs.com/benefits), by phone (1-888-628-2770 (TTY 711), or pick up at any CVS Pharmacy.
Certain DME supplies are medical benefit only. If your pharmacy wishes to dispense DME supplies (nebulizers, etc.) via medical benefit, please contract with our plan by completing the contract request form found here: https://www.oklahomacompletehealth.com/providers/become-a-provider.html
Oklahoma Complete Health is expanding the prescription benefit to improve access to care. Beginning April 1, 2025, medications across five (5) drug classes will not count towards the member’s monthly six (6) prescription limit.
The drug classes are as follows and include more than 500 medications.
Systemic Antibiotics and Antivirals
Anticonvulsants
Behavioral Health Medications
Cardiovascular Medications
Diabetic Therapies
This prescription enhancement will help reduce ER visits and readmissions, while lowering members’ out-of-pocket costs and reducing wait times for medication refills.
For claims processing assistance, please call our pharmacy helpdesks (open 24/7) at 1-833-750-3660 (SoonerSelect) or 1-833-750-3682 (Children's Specialty Plan).
General questions or escalations can be directed to: oklahoma_complete_health_pharmacy@centene.com
Oklahoma is participating in the CMS CGT-CMMI Model for Casgevy & Lyfgenia. See below for supporting information for our billing providers:
- Provider Billing Instructions:
- Casgevy & Lyfgenia are on OHCA’s hospital carve out list . Both medications require prior authorization (PA) and are reviewed via medical benefit only. Criteria for both medications are found here: OHCA Criteria (This is an external link that will take you outside the Oklahoma Complete Health website).
- Submit medical PA via Availity (This is an external link that will take you outside the Oklahoma Complete Health website). All medpharm/buy & bill pharmacy PA’s will be reviewed/determined within 24 hours of receipt.
- If PA approved, & member has been treated and discharged, the billing provider should:
- Submit inpatient or outpatient claim separate from carve out drug claim via OCH secure web portal (This is an external link that will take you outside the Oklahoma Complete Health website).
- Carve out drug claim should include appropriate HCPCS code, NDC, purchase invoice, applicable 340B modifier
- Casgevy (exagamglogene autotemcel): NDC 51167-0290-09, Procedure Code: J3392
- Lyfgenia (lovotibeglogene autotemcel): NDC 73554-1111-01, Procedure Code: J3394
- Providers may not use 340B discounts on model drugs; therefore, 340B providers should utilize modifier UD for Casgevy & Lyfgenia
- A provider who submits a claim for administration of a State-Selected Model Drug must be a member of the CMS-designated patient registry for the Model and participate in a CMS-specified study. Participating Centers
- For additional guidance please refer to our provider billing manual
- Primary and secondary point of contact for providers regarding single case agreements, PAs, and provider enrollment:
- Contracting:
- Contract Request Form
- Is OCH currently contracted with any of the treatment centers authorized to administer Casgevy and Lyfgenia gene therapy?
- Yes, Children’s Medical Center of Dallas/Plano
- Single Case Agreements can be created as needed for alternative authorized treatment centers
- Continuity of Care:
- We ensure continuity of care for Candidate and Model Beneficiaries that switch between FFS and managed care, or among MCPs within the state, including honoring prior authorizations for SCD gene therapy-related care and prescriptions
- We ensure that Model Beneficiaries continue to have access to their same SCD gene therapy providers until at least one year after receiving their gene therapy infusion. We have the ability to adjust the length of care within each SCA agreement.
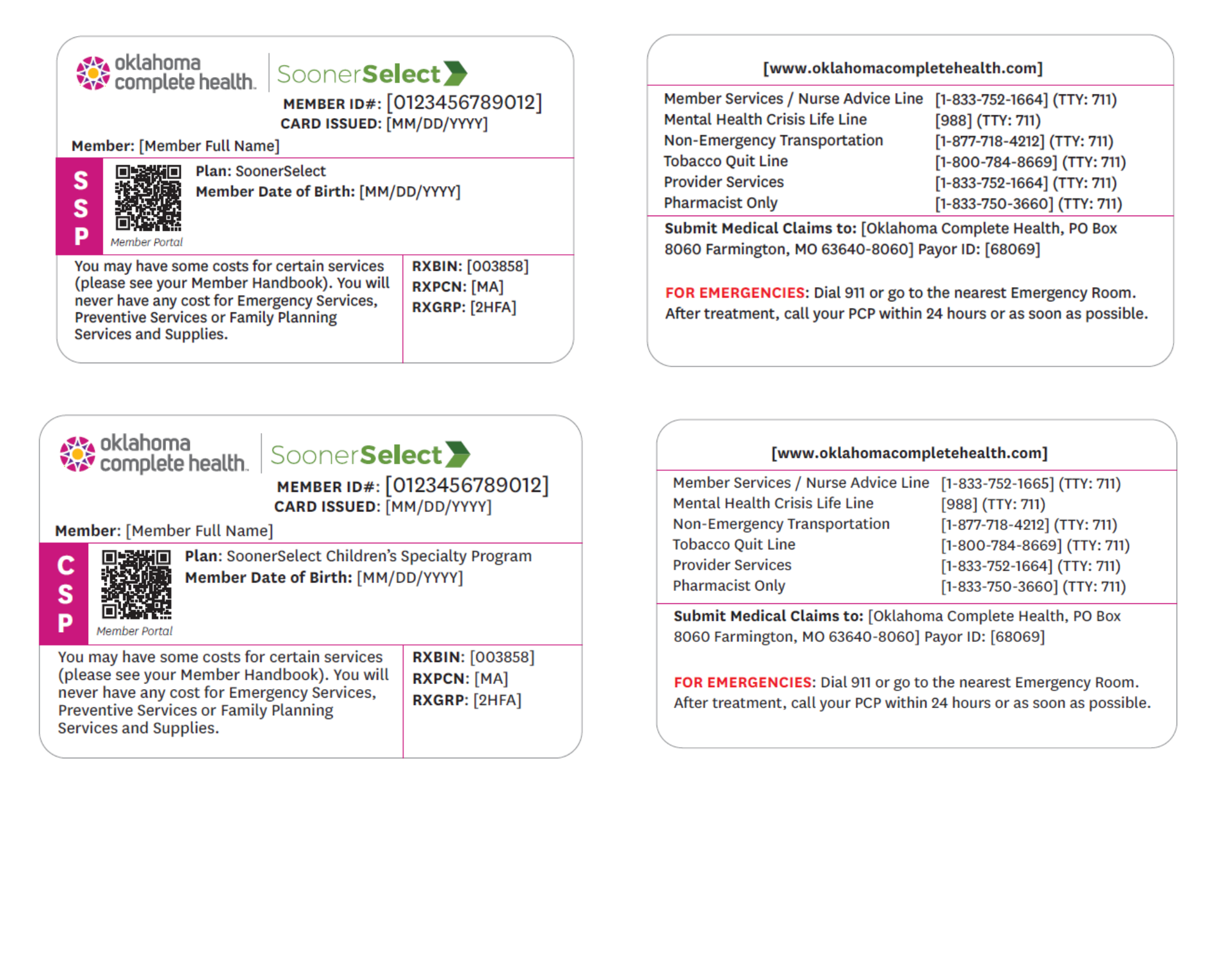
Example ID Cards
Please call member, provider, or pharmacy services for all patient related inquiries. Phone numbers differ for Sooner Select (SSP) and Children's Specialty Programs (CSP). Important numbers can be found on the back of your member ID Card.